Lumity’s mission to deliver a superior benefits experience by clarifying benefits for employers and employees started out with our founder’s frustration with purchasing and using employee benefits, both at a corporate level and at an individual level when his wife came down with an illness.
When it came to choosing the right plan during enrollments, the question was: “How do I know which plan is right for me?”
As we asked employees from all walks of life, it became apparent that technology (and data) could answer the four critical questions that provided the best answer to this very frustrating employee enrollment process.
1. Are my doctors in-network?
Lumity’s carrier integrations help determine this for the employee. By providing a 5-7 year lookback on an employee’s doctors / providers, an employee going through Lumity’s enrollment portal today can ensure this question is answered.
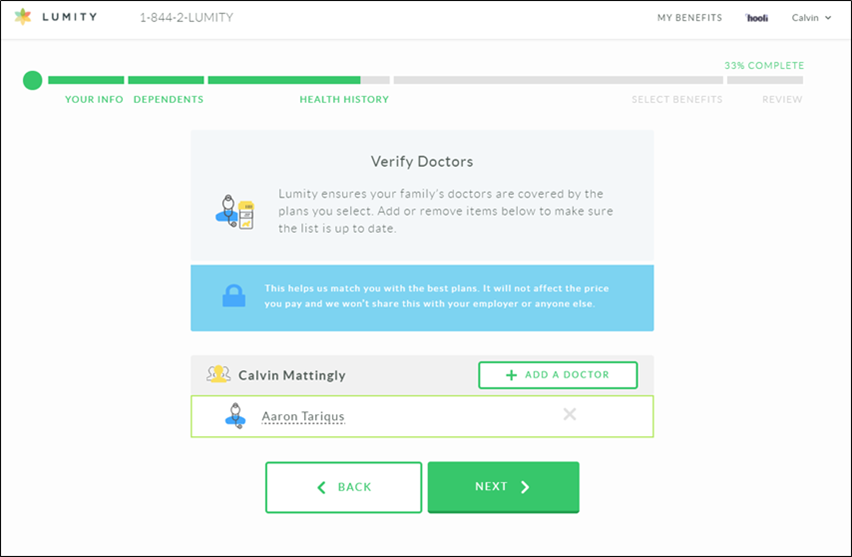
2. Are my prescriptions in formulary?
Similarly, an employee can select their active prescriptions to ensure they are in the carrier’s formulary. The 5-7 year lookback will ensure all active prescriptions are included, giving the employee the option of selecting active, ongoing prescriptions.
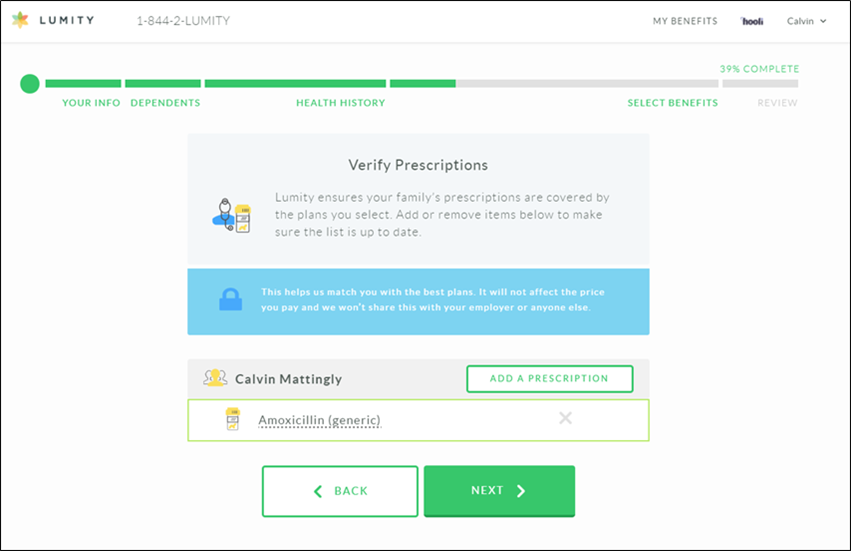
3. How much am I expected to pay next year in healthcare costs?
We crunch the data in real-time, calculating an expected cost of healthcare for each employee, in order to drive a personalized recommendation for each employee enrollment (and/or their dependents).
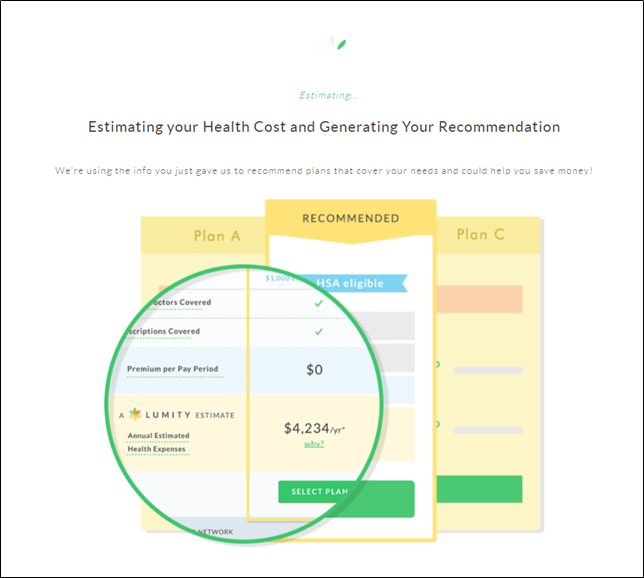
4. Based off my expected needs (and/or those of my dependents), which plan is the best value?
The value (not cost)-driven recommendation is tailored to each employee based on their unique needs. For a young, healthy employee (example below), a high deductible plan with an employer-sponsored HSA contribution may be the best option.
Similarly, for an employee who has a higher health risk profile, a lower deductible PPO or HMO may be a better fit, depending on preference. The guiding philosophy is not to force a choice, but to provide a data-driven recommendation.
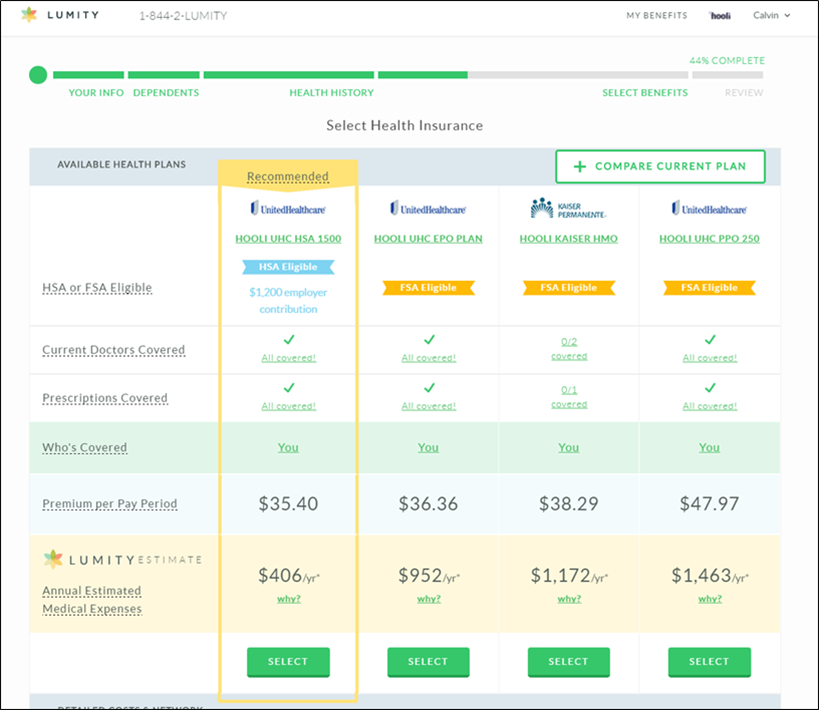
Given the current layout, Lumity’s clients have seen HSA adoption rise from 5% to upwards of 50% or over. The data-driven recommendation for employees completes the benefits lifecycle, optimizing for the right plan given the specific needs of each employee, preventing over or under-coverage relative to needs.
To understand how we partner with employers to determine the right benefits package for the employee population, download our e-book or just fill out the form below and we'll get in touch.
Schedule a Free Consultation Now.
