At around 250 employees, your company should be getting your medical claims from your broker or carrier. This claims visibility is a good start to understanding your healthcare costs, but this is just the first step. The real key to managing costs lies in what your broker does with your data.
A Data-Driven Benefits Program
The real cost control comes with claims analytics—because the devil's in the details. With a data-driven benefits program, it's possible to know:
- How your claims performance trends over time with your expected loss ratio, and
- How your large claims fit into your total claims expense.
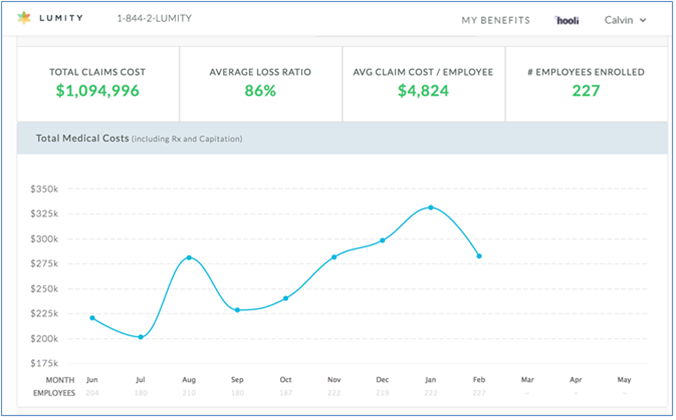
Why is claims performance important?
Claims performance is indicative of whether your company is running well or running "hot." If the claims performance is running over the expected trend, your team should anticipate and forecast higher per employee benefits costs for the coming plan year.
On the other hand, if it's lower than expected, you may be able to realize significant savings and/or reallocate budget towards employee wellness initiatives.
How does this help me manage renewals?
As a data-driven benefits broker, Lumity brings claims analytics to the table when we negotiate with carriers on your behalf. Data levels the playing field, so you get a fair and transparent renewal.
Additionally, lower-than-expected claims can deliver further savings. A level-funded company may get a rebate for coming in below the carrier's expected medical loss ratio (MLR).
You'll also know when it's the right time to move to self-funded.
