If your 2025 benefits renewal felt unusually difficult to navigate, you were not alone—and more importantly, it wasn't random.
I've had the same conversation with dozens of leadership teams recently: "We knew costs were going up… but not like this." Renewals didn't just increase this year—they felt sudden, hard to explain, and even harder to control.
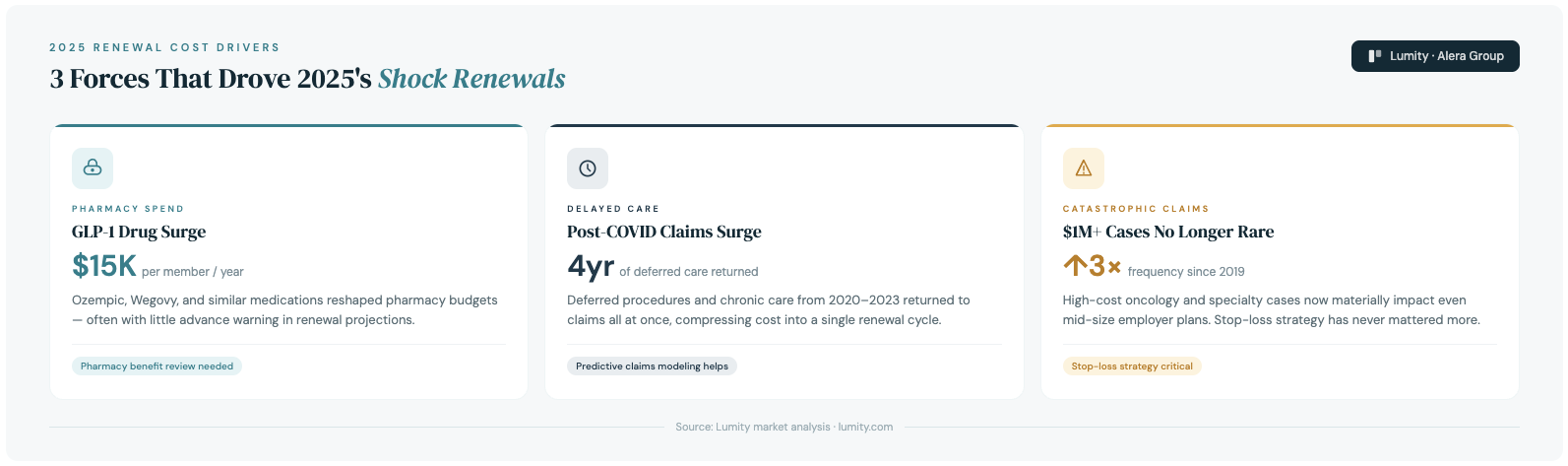
The biggest drivers were consistent across the market. GLP-1 medications like Ozempic and Wegovy rapidly reshaped pharmacy spend, often exceeding $10,000-$15,000 per member annually 💊. Delayed care from the COVID era returned all at once 🏥. High-cost claims—especially $1M+ oncology and specialty cases—are no longer rare ⚠️.
Regulatory and compliance pressures have added further complexity, leaving many employers managing more variables without better insight into what is driving cost.
The real issue is structural. Most companies still treat renewal as a once-a-year event. By the time options are reviewed, outcomes are largely set. The teams that felt more in control approached things differently. They started earlier, monitored claims trends, modeled decisions in advance 📊, and explored alternative funding strategies.
Looking ahead to 2026, these pressures remain. But the difference is timing and clarity. Organizations that act early will have something most lacked going into 2025: options.

You still have time to engineer a better outcome for 2026. At Lumity, we help teams pressure-test strategy and uncover opportunities—even if they ultimately stay the same.
About the Author
Casey Wetzel, Director of Business Growth at Lumity, an Alera Group Company, is a licensed employee benefits advisor specializing in helping organizations design scalable, cost-effective benefits strategies. She partners with HR and finance leaders to improve visibility into healthcare spend and drive more informed decision-making.
